This article is for informational purposes only and is not a substitute for medical diagnosis. If tongue lesions persist for more than a few days, it is recommended that you see a dentist or oral surgeon!
Proboil ® is the ideal choice for gentle yet effective cleaning of the tongue and tongue cavity, as it contains only mild, natural ingredients.
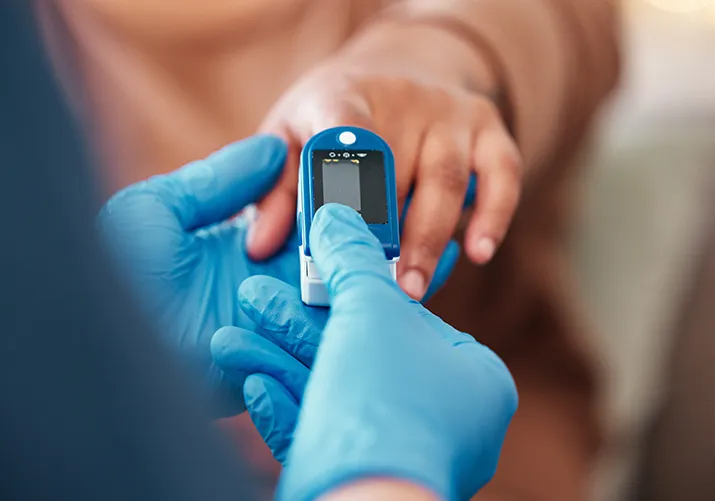
Diabetes: how it affects your gums and oral health
Blood sugar control plays a key role not only in protecting your internal organs, but also in the health of your oral cavity. Impaired glucose metabolism—whether hidden or already diagnosed as prediabetes or diabetes—can seriously increase the risk of gingivitis and other oral inflammations. But why does this happen, and what can you do about it?
In this article, we will take a simple yet scientifically sound look at how sugar metabolism affects oral health and why it is worth paying special attention to prevention.
What is a sugar metabolism disorder?
Sugar metabolism disorders include prediabetes (elevated fasting blood sugar levels), insulin resistance, and type 2 diabetes. These pathological conditions refer to an imbalance in metabolism, when the body is unable to properly regulate blood sugar levels.
Although most people associate diabetes with eye, kidney, or heart disease, few people know that the oral cavity is one of the first areas where symptoms can appear.
Insulin resistance: a hidden risk factor behind oral inflammation
Many people are unaware that insulin resistance (IR) is often behind glucose metabolism disorders—a metabolic disorder in which the body’s cells are less sensitive to the effects of insulin. This condition can not only lead to fluctuations in blood sugar levels, but can also create a basis for the development of various inflammatory processes, including in the oral cavity. Higher blood sugar levels and a weakened immune response can lead to more frequent gum bleeding, gum inflammation, or even periodontal disease. This is why early detection and treatment of insulin resistance is important—not only to protect internal organs, but also to maintain oral health.
The link between sugar and gingivitis
Elevated blood sugar levels can trigger inflammatory processes in the body, including in the mouth. Chronically high glucose levels:
- weaken the immune system,
- promote the growth of bacteria in the mouth,
- slow down wound healing,
- and increase susceptibility to inflammation.
This is why gum bleeding, gum swelling, and periodontal disease are more common among diabetics. After a while, inflamed gums are no longer able to properly adhere to the teeth, which can lead to gum recession, tooth loss, and even tooth loss if left untreated.
The close relationship between oral inflammation and blood sugar
An interesting duality can be observed: high blood sugar levels promote the development of oral inflammation, while untreated gum inflammation can also raise blood sugar levels. This is a vicious cycle that is difficult to break unless both problems are treated simultaneously.
Several studies have shown that properly treated gum disease—such as professional tartar removal and a targeted oral hygiene routine—can reduce HbA1c levels, which is an important indicator of long-term blood sugar levels.
What symptoms may indicate a glucose metabolism disorder in the mouth?
- Frequent gum bleeding when brushing or chewing
- Unpleasant mouth odor that does not go away even after using mouthwash
- Gum swelling, sensitivity, pain
- Dry mouth (due to reduced saliva production)
- Slow wound healing in the mouth (e.g., after canker sores or bites)
- Unpleasant feeling around the teeth, mobility
If you experience these symptoms, it is worth visiting not only your dentist, but also your family doctor or diabetologist, as these may be early signs of a more serious metabolic disorder.
How can you protect your oral health if you have diabetes?
- Regular dental check-ups
- It is advisable to have your teeth and gums checked at least every six months, especially if you have already been diagnosed with diabetes.
- Targeted oral care
- Professional help is usually needed to learn effective oral care. Maintaining impeccable oral hygiene at home is essential. Proper brushing technique, cleaning of interdental spaces and gum lines according to individual characteristics, and regular toothbrush replacement. Your dentist will determine the frequency of professional teeth cleaning and regular dental check-ups.
- Stabilizing blood sugar levels
- Dietary changes, exercise, and, if necessary, medication are essential to reduce the body’s susceptibility to inflammation, including in the mouth.
- Avoid smoking
- Smoking further aggravates gum inflammation and impairs wound healing. Quitting smoking significantly improves the health of the oral cavity.
Did you know? Gum inflammation is not just an aesthetic problem
Inflamed gums are not only unpleasant and painful, but can also have serious long-term consequences. Inflammatory foci in the mouth can affect the entire body and are associated with cardiovascular disease, premature birth, and even Alzheimer’s disease. Prevention is therefore in the interest of not only your mouth, but your entire body.
When should you see a doctor?
If your gums bleed regularly, are swollen or receding, or you have bad breath, don’t wait! Early diagnosis and treatment are crucial in preventing complications, both dental and metabolic.
+1 tip: Support your oral flora from within
The health of your oral flora is closely related to the condition of your intestinal flora. Ingredients that keep the gut microbiome in balance can also have a positive effect on the oral cavity’s defenses. That’s why, in addition to a healthy diet, it’s a good idea to take complex supplements that support both gut flora and oral health.
Proboil® is an innovative mouthwash that helps maintain the balance of oral flora and intestinal flora with its live flora and vitamin content, thus contributing locally and internally to maintaining the health of the gums and teeth. Regular use is especially recommended for those who suffer from diabetes or are prone to oral inflammation.
Important note
This article is for informational purposes only and is not a substitute for medical diagnosis or treatment. If you suspect symptoms of diabetes or experience frequent gum inflammation or inflammation of the oral cavity, be sure to consult your family doctor or dentist.
Proboil® can be an ideal addition to your oral care routine if you have a metabolic disorder, as its natural ingredients gently support the balance of oral flora, helping to prevent inflammation.